The Dutch Society of Physical Therapy (KNGF) criticized the manipulative assessment and treatment approach of the Craniofacial Therapy Academy (CRAFTA) education and rejected more than 50 % of the possible accreditation points..
In the Netherlands the accreditation commission of the Dutch Society of Physical Therapy (KNGF) criticized the manipulative assessment and treatment approach of the Craniofacial Therapy Academy (CRAFTA) education and rejected more than 50 % of the possible accreditation points which were supposed to be credited to post graduate physical therapist.
No accreditation points at all were awarded to the manual therapist. The leading reason of this decision was that “The techniques which are used are osteopathic techniques and are not evidence based. The techniques are NOT based on western rationales. “. The names of the members of the accreditation commission, who are also physical therapists, are not named by the Dutch association of physical therapy (KNGF). Hence, a fair and open discussion was not possible. Therefore, we see this blog as an opportunity to explain cranial manual therapy.
What is cranial manual therapy?
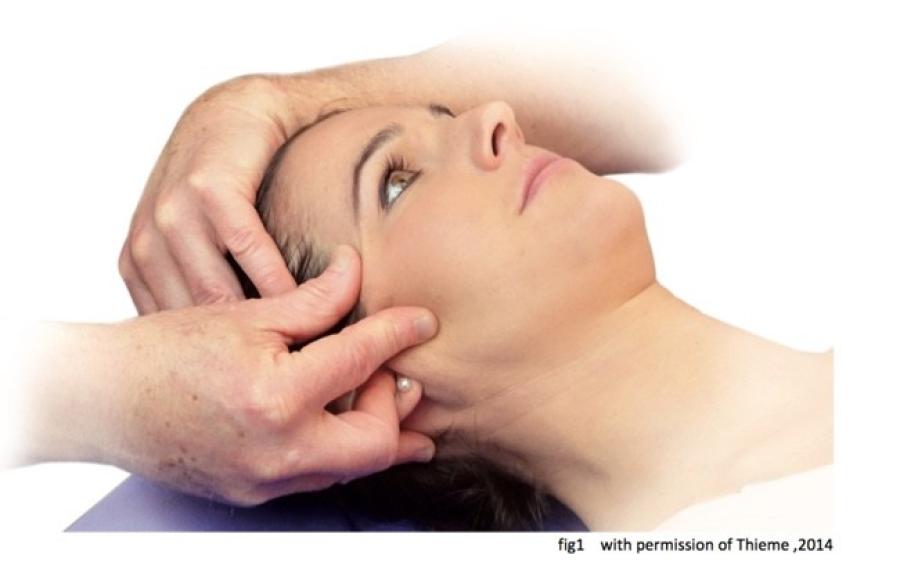
In the CRAFTA® education cranial manual therapy means: assessment and treatment of the cranium (head) and the face with passive movements (movements executed by the therapist). During the examination three parameters are examined: resistance, rebounce and sensory response.
- Resistance: is the start and the quality of the pressure, which is analyzed during the increased pressure of the passive movements (Maitland et al 2013)
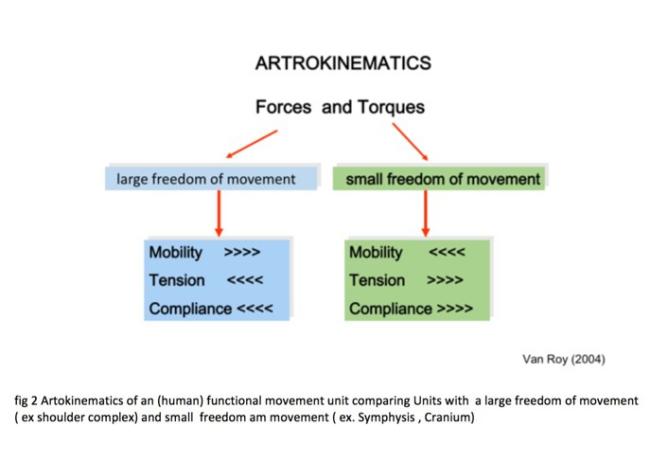
- Rebounce: a reaction of the cranial bone tissue by decreasing tension executed by an external force like a passive movement. This reaction is based on the cranial architecture and the transducing of forces between the bone structures. These are called stresstransducer system (Oudhof 2001, Proffit 2013 ).
- Sensory response: the personal experienced by the patient during performing of cranial passive movement, e.g. pain, dizziness, tinnitus, heavy body feeling and others.
These three parameters will first be examined through six standard tests. In the following, specific regional tests, related to the findings out of the six standard tests, can be performed. Abnormal findings like increased resistance, reduced rebounce or the reproduction of the patient’s symptoms (sensory responses) may provide information or clues, supporting clinical patterns. These clinical patterns might stem from, e.g. post–traumatic headache, a unilateral subjective tinnitus, face trauma, chronic (pseudo) sinusitis or paediatric ear pain.
The parameters are based on the evidence from cranial growth models and research out of the scientific fields of orthodontics, plastic and neural surgery (Smith and Josell 1986, Proffit 2013) and the latest pathobiological knowledge from pain science and the innervation of cranial tissue (Schueler et al 2013).
What is the difference between cranial manual therapy (CM) and craniosacral therapy (CS)?
There is strong clinical evidence that cranial passive movements may change complaints and function in human beings. For an excellent overview about different models it is referred to Chiatiow , Cranial Manipulation . Theory and Practice” (Chiatow 2005). Most of them are driven by the cranial sacral rhythm. This is a cyclic movement of all body tissue related to the movement of the spinal fluid. It is called the primary respiratory mechanism.
- CM is based on growth studies coming from the fields of orthodontics, plastic and neuro surgery. This is in contrast to the ideas of CS and the primary respiratory mechanism.
- CS is based on biomechanical/anatomical models. CM is orientated on functional/biological/ pragmatic models.
The treatment goals are different
- – CM assessment and management techniques look for clinical signs(Resistance, Rebounce, and Sensory Response). CS is very focused on changes in structures and systems (suture, ventricle, psycho-emotional systems).
- – CM always combines craniofacial functions like for example eye movements,respiratory and tongue exercises/ training. CS stays passive because of the “self-healing’ mechanism of the body.
Cranial manual therapy aims not……
- to mobilize sutures, as it is known from studies that several kilograms are needed to achieve minimal sutural movement (Downey et al 2005)
- to push out ventricles and to base the effects on the cranial sacral rhythm due to the lack of evidence ( Sommerfield et al 2004 )
- to leave the patient passive with a “wait and see” approach after the treatment
Cranial manual therapy aims to …
- Carry out a systematic analyses of the abnormal tension in the cranial bones related to the patient’s complaints, which are expressed in three parameters (resistance, rebounce and sensory response). It is based on pain mechanisms and classification of pain ideas.
- Support biological function of the cranial tissue during growth and to reduce (multiple minor) nociception in the craniofacial area. Further, it aims to restore its function (normal stress-transducing ) and to stimulate craniofacial organ functionsIs there evidence for cranial manual therapy?
It is advocated that stress and strain function of cranial bones maybe influenced by craniofacial (dys-) functions (Gabutti and Draper 2014).
Further, it is stated that pericranial tissues can directly influence meningeal nociception associated with symptoms like headache ( Schueler 2014). However, a systematic effect study based on this background is lacking. In a systematic review by Krützkamp et al (2014) about the outcomes of the treatment of the craniofacial tissue by passive movements, 37 studies were identified related to orthodontic splint therapy, craniosacral or manual therapy as passive interventions. All had a poor methodological quality and small groups. Only very little evidence could be identified concerning the outcome of all therapy approaches on headaches and psychogenic problems.
Maybe the accreditation commission of the Dutch Society of Physical Therapy is correct in stating, that there is a lack of direct scientific evidence, which comes out of effect studies. However, empirically gathered knowledge by therapist, patients and external evidence from other disciplines help to better understand the function of the craniofacial region. Further, this knowledge supports the cranial manual therapy model which is clearly NOT the same as craniosacral therapy.
If you have experience as a patient with cranial manual therapy as it is performed in the CRAFTA® education or as a therapist, please comment on this blog and share your experiences. This may help to better understand cranial manual therapy and may support helping patients who suffer from long term head- and face problems.
Kind Regards Harry von Piekartz
References:
- Chiatow L , Cranial Manipulation Theory and Pracrice , 2 nd Edition, 2005, Elsevier , Chruchil Livingstone , Edinghburgh
- Downey PA1, Barbano T, Kapur-Wadhwa R, Sciote JJ, Siegel MI, Mooney MP. Craniosacral therapy: the effects of cranial manipulation on intracranial pressure and cranial bone movement. J Orthop Sports Phys Ther. 2006 Nov;36(11):845-53.
- Gabutti, M ,Draper-Rodi J Osteopathic decapitation: Why do we consider the head differently from the rest of the body? New perspectives for an evidence-informed osteopathic approach to the head International Journal of Osteopathic Medicine (2014) 17-23
- Krützkamp L, D Möller, von Piekartz H. Influence of Passive Movements to the Cranium systematic Literature review. Manuelle Therapie 2014; 18: 183–192Maitland G, Hengeveld E, Banks K, English K. Vertebral manipulation, 6th ed. Oxford: Butterworth-Heinemann; 2013
- Oudhof H. Skull growth in relation to mechanical stimulation. In: von Piekartz H, Bryden L. Cranialfacial Dysfunction and Pain, Assessment, Manual Therapy and Management. Oxford: Butterworth-Heinemann; 2001
- Proffit WR. Contemporary Orthodontics. 5nd ed. St. Louis: Mosby Year Book; 2013
- Schueler M1, Messlinger K, Dux M, Neuhuber WL, De Col R. Extracranial projections of meningeal afferents and their impact on meningeal nociception and headache Pain. 2013, Sep;154(9):1622-31
- Sommerfeld P1, Kaider A, Klein P. Inter- and intraexaminer reliability in palpation of the “primary respiratory mechanism” within the “cranial concept”. Man Ther. 2004Feb;9(1):22-9
- Smith R, Josell The plan of the human face: a test of three general concepts. Am J Orthod. 1984 Feb;85(2):103-8.
For further reading:
 Craniofacial Pain
Craniofacial Pain
Neuromusculoskeletal Assessment, Treatment and Management. 2007 Elsevier ISBN: 978-0-7506-8774-4
